Synexis Technology Advantage in Healthcare Environments


Cleaner Privacy Curtains & Other Hard-to-Reach Surfaces
Complements EVS Work
Supports Healthier Conditions for Staff
Mitigates Odors in
Long-Term Care Facilities
Elevates Standard of Care &
Supports Patient Satisfaction
Supports Infection
Control Risk Assessment
(ICRA) Strategy
Cleaner Privacy Curtains & Other Hard-to-Reach Surfaces
Complements EVS Work
Supports Healthier Conditions for Staff
Mitigates Odors in
Long-Term Care Facilities
Elevates Standard of Care &
Supports Patient Satisfaction
Supports Infection
Control Risk Assessment
(ICRA) Strategy
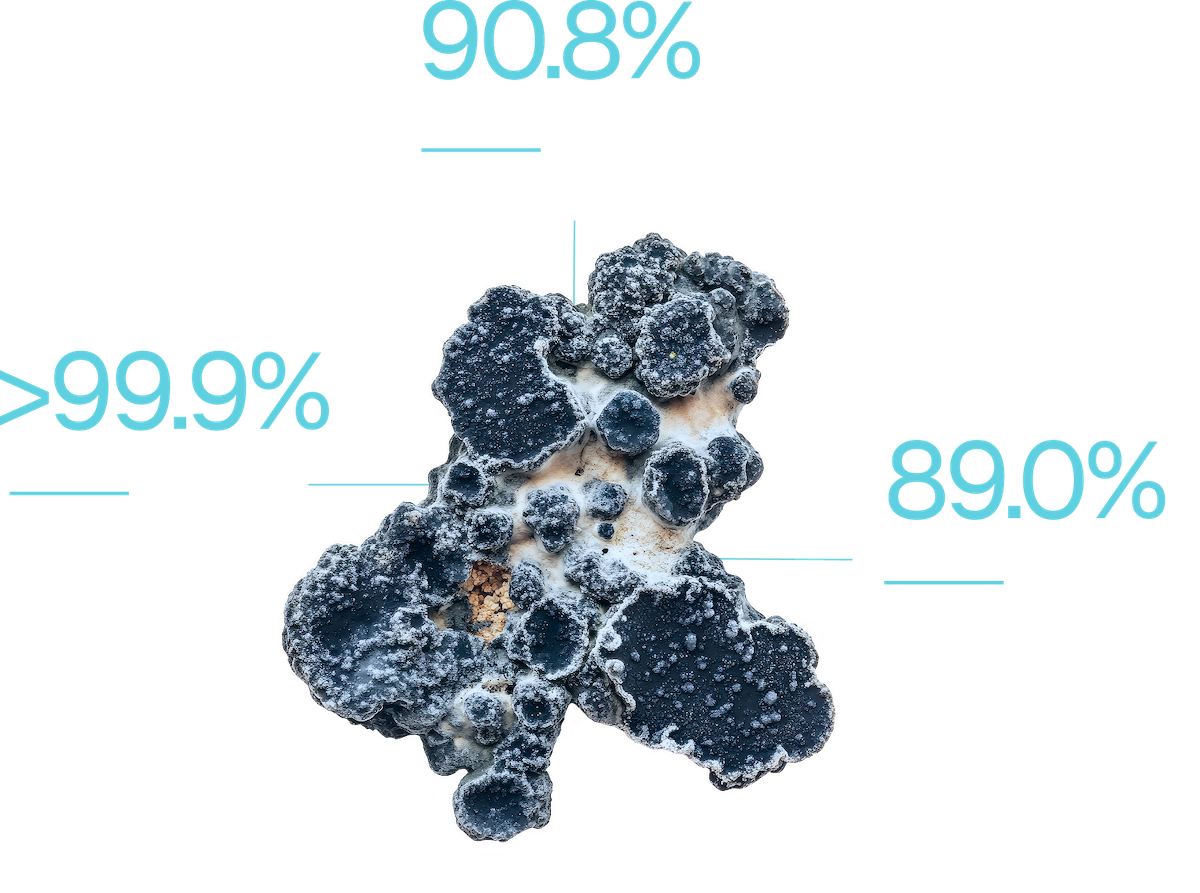
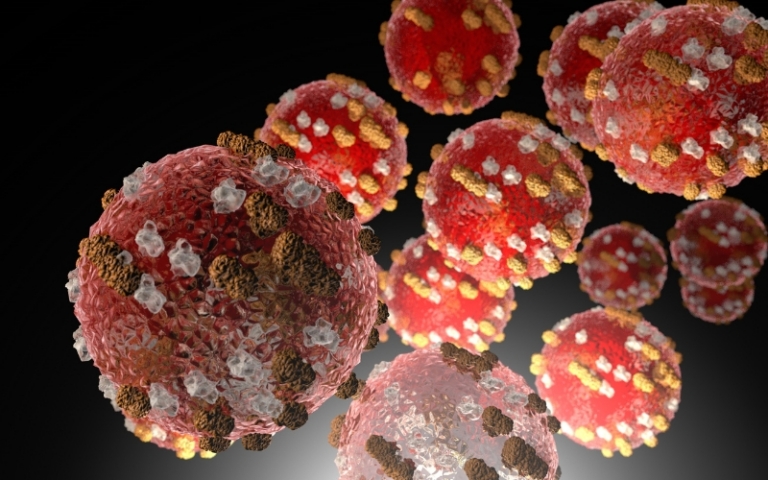
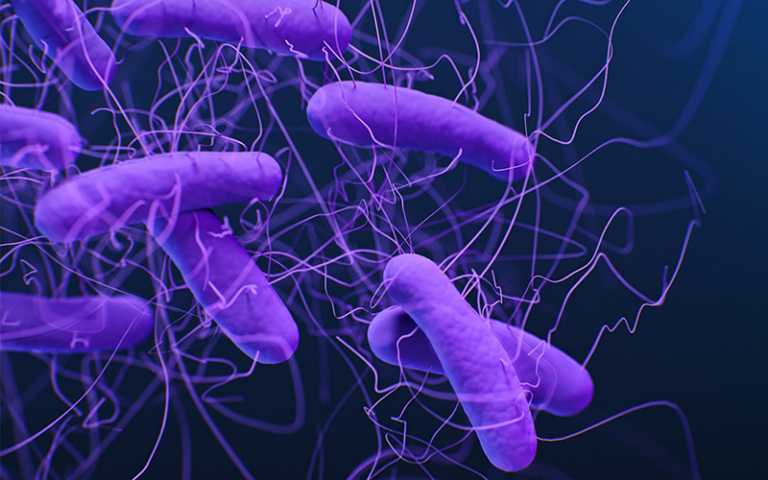
Reducing Surface-Level and Airborne Pathogens
Card 1
Continuous,
& Proactive
Pathogen
Control
Card 1
Continuously reduces harmful pathogens in the air and on surfaces, supporting infection prevention strategies in patient rooms, surgical suites, common areas, and more.
OSHA-compliant* and aligned with CDC and EPA guidelines for continuous use in occupied spaces.
Card 2
Odor Control
Card 2
Reduces persistent odors from the environment, antiseptics, disinfectants, and medical waste, all without masking agents or added fragrances.
Synexis DHP® is odorless and designed for sensitive healthcare environments.
Card 3
Experience for
Patients, Staff
& Visitors
Card 3
Supports a more comfortable, confidence-building healthcare experience by continuously reducing pathogens and odors in the background.
With quiet, touchless operation, Synexis DHP® technology helps create a safer, healthier environment for staff, patients, and visitors—without interrupting vital care.
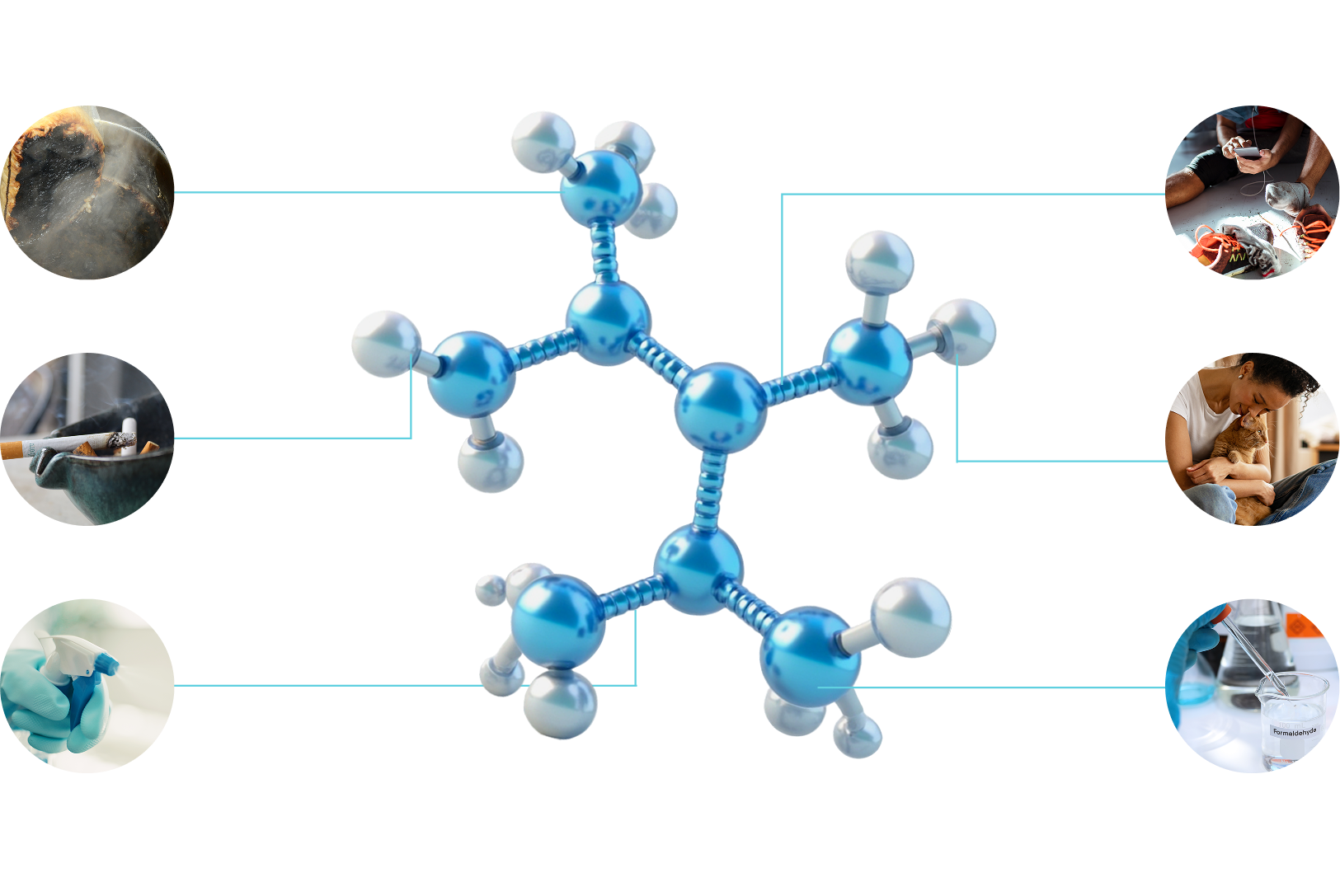
How Synexis Technology Works
Our patented technology transforms ambient oxygen and humidity in the air into DHP®, which flows freely and continuously to reduce the presence of viruses, bacteria, fungi, and volatile organic compounds (VOCs) on surfaces and in the air. Synexis offers in-duct and stand-alone devices for scalable deployment options from small rooms to larger indoor facilities.
Why Do Healthcare Facilities Choose Synexis?
Preventing just one healthcare-associated infection (HAI) could save your facility tens of thousands in treatment costs, penalties, and reputation management, likely for less than the investment in Synexis technology.
Pathogen Control with the Sphere Device
Easily placed or mounted where needed, the Sphere runs on a standard outlet and blends into any environment. Its adaptable design ensures targeted treatment in key zones of interest.

the synexis sphere